Uterine lining overgrowth: what it is and what to watch for
Uterine lining overgrowth, often called endometrial hyperplasia, means the tissue that lines your uterus has gotten thicker than it should. That happens when estrogen and progesterone fall out of balance or when the lining doesn’t shed regularly. It’s not the same as cancer, but some types can raise your chance of developing endometrial cancer later on. Knowing the signs and next steps helps you act fast.
Causes and common symptoms
Many things can push the uterine lining to grow too much. Hormone imbalances from PCOS, obesity, certain hormone therapies, and some fertility drugs are common causes. Tamoxifen, a breast cancer drug, can also trigger overgrowth. Women who don’t have regular periods—either from menopause or anovulation—are at higher risk.
Symptoms are often easy to spot: heavier or longer periods, spotting between cycles, or any bleeding after menopause. Some people feel pelvic discomfort, but often there are no pain symptoms. If you notice any unusual bleeding, don’t ignore it—get checked.
How doctors check and treat it
Your clinician will usually start with a pelvic exam and a transvaginal ultrasound to measure the lining’s thickness. If the lining looks thick or if bleeding is unexplained, an endometrial biopsy or hysteroscopy gives tissue for testing. That tells whether cells are simple overgrowth or show atypia—meaning abnormal cells that need closer follow-up.
Treatment depends on the type and your goals. For simple overgrowth without atypia, a course of progestin usually calms the lining and can reverse changes. Progestin can be given as a pill, injection, or with a hormonal IUD (like Mirena), which often works well and limits systemic side effects. If biopsy shows atypical cells or if medication doesn’t work, a hysterectomy may be recommended—especially if you don’t want more children.
There are less major options too: a dilation and curettage (D&C) can remove excess tissue and help both diagnose and treat. After treatment, follow-up scans or repeat biopsies are common to make sure the lining returns to normal.
Fixing underlying issues helps prevention. Losing weight, treating insulin resistance or PCOS, and reviewing hormone therapy with your doctor cut the risk. If you’re on tamoxifen, ask your oncologist about monitoring plans.
Bottom line: odd bleeding is the main red flag. If periods change or you have postmenopausal bleeding, book an appointment. Early checks and the right treatment usually fix the problem and lower future cancer risk.
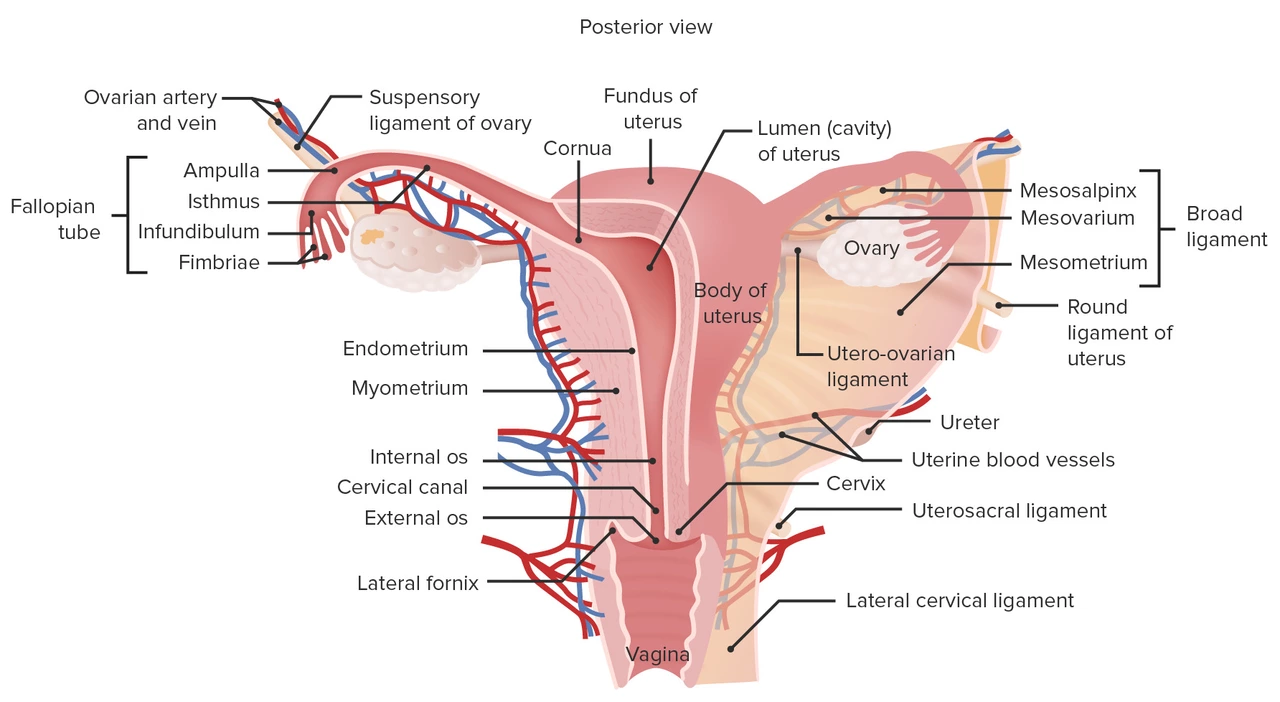
The Role of Endometrial Hyperplasia in Overgrowth of the Uterine Lining
- May, 6 2023
- Daniel Remedios
- 18 Comments
As a blogger, I've recently been researching the role of endometrial hyperplasia in the overgrowth of the uterine lining. Endometrial hyperplasia is a condition where the uterine lining thickens, which can be caused by an imbalance of hormones, particularly estrogen. This thickening can lead to heavy or irregular periods, and in some cases, can even cause infertility. It's important to monitor and treat endometrial hyperplasia, as it may increase the risk of developing uterine cancer. Overall, understanding and addressing endometrial hyperplasia is crucial for maintaining a woman's reproductive health.
