Tests: What Labs and Checks You Actually Need for Medicines and Supplements
Starting a new drug or supplement? Tests tell you if it’s safe and working. This tag collects easy-to-follow advice about which labs to get, when to repeat them, and which signals mean you should call your doctor. You'll find practical notes tied to common meds—from Depakote and statins to diabetes drugs, blood thinners, and fertility treatments.
Common lab tests to know
Before you begin many medicines, a baseline helps. For example, Depakote often needs liver enzymes and a complete blood count to watch for liver injury or low platelets. Statins like Crestor start with a lipid panel and a liver enzyme check. Metformin and several diabetes drugs require a kidney function test (eGFR) so your dose is safe. Diuretics such as Lasix affect electrolytes and kidney numbers, so clinicians monitor sodium, potassium and creatinine.
Blood thinners differ. Warfarin needs INR monitoring, while dabigatran usually does not—yet kidney function matters because the drug clears through the kidneys. Naltrexone (Revia) can stress the liver, so a baseline liver panel is smart. Fertility meds? Pregnancy tests and hormone checks guide timing and safety. If a drug has known blood-level monitoring (some antiepileptics, valproate levels), ask your prescriber how often to measure.
Testing when buying meds online and staying safe
Ordering from online pharmacies is convenient but adds steps. First, verify the pharmacy’s credentials and read safety guides before purchasing—fake sites sell dangerous or ineffective products. When you buy meds online, keep copies of your lab results and prescriptions in cloud storage so a new provider can review them quickly.
If you switch suppliers or try alternatives like different blood pressure or antidepressant options, retest relevant labs after a few weeks to make sure the new drug suits you. For weight-loss drugs or GLP-1 alternatives, monitor blood sugar, kidney function, and symptoms like dizziness or rapid heart rate. For antibiotics or herbal supplements, watch for new allergies, liver changes, or interactions with current meds.
Practical steps you can use tomorrow: ask your clinician for a baseline lab set before starting any new prescription; request written guidance on which numbers will trigger a dose change; schedule the first follow-up lab within 4–12 weeks depending on the medicine; and keep a simple record of results and symptoms.
If you want quick reads, check tag articles on lab needs for Depakote, Crestor, diabetes medications, dabigatran risks, and online pharmacy safety. These posts give condition-specific checks and red flags so you can act fast if something looks off.
Know urgent red flags: sudden jaundice, dark urine, unexplained bruising, severe muscle pain, fainting, shortness of breath, or fever with a new drug. If you notice any of these, stop the medicine and contact emergency care or your prescriber right away. Keep a simple list of your current drugs and recent lab dates in your phone so any clinician can act fast. Small prep like this prevents big problems.
Browse these posts and bookmark tests you need today.
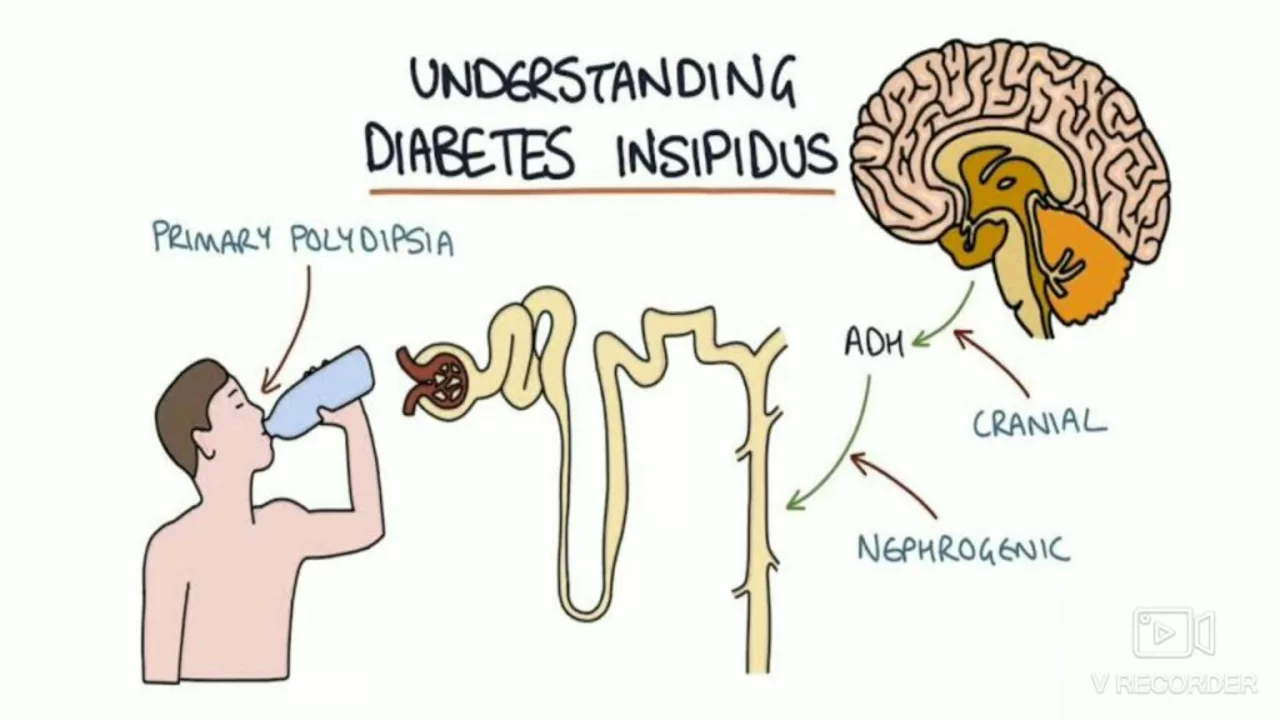
Diagnosing Central Cranial Diabetes Insipidus: Tests and Procedures
- Jul, 1 2023
- Daniel Remedios
- 16 Comments
In my recent exploration, I focused on the diagnostic processes involved in identifying central cranial diabetes insipidus. I found that doctors often perform blood and urine tests initially to check for low sodium levels and high urine output. Water deprivation tests and MRI scans are also used to confirm the diagnosis and assess the pituitary gland's condition. Desmopressin tests can then help to distinguish between central and nephrogenic diabetes insipidus. It's a detailed process, but crucial for ensuring accurate diagnosis and treatment.
