Endometrial hyperplasia — what you need to know fast
If you’ve had heavier or irregular periods, spotting after menopause, or pelvic pain, endometrial hyperplasia could be the reason. It happens when the lining of the uterus (the endometrium) gets thicker than it should. That thickening is usually from too much estrogen acting without enough progesterone to balance it. Some types are low risk, others can turn into cancer if left untreated — so spotting the problem early matters.
Common causes and who’s at risk
Think of estrogen as the growth signal for the uterine lining. Causes that raise estrogen or lower progesterone include obesity, polycystic ovary syndrome (PCOS), hormone replacement therapy without progesterone, anovulatory cycles (no ovulation), and certain fertility drugs. Tamoxifen, a breast cancer drug, can also increase risk. Women approaching menopause and those with irregular cycles are more likely to notice symptoms.
Age, weight, and medical history matter. For example, many readers here exploring fertility and ovulation topics will recognize PCOS as a linked condition. If you’ve been treating infertility or using ovulation drugs, mention that to your provider — it changes how they look for endometrial issues.
Signs, tests, and what to expect from diagnosis
Most people notice abnormal uterine bleeding: heavier periods, longer periods, bleeding between cycles, or any bleeding after menopause. Your doctor will usually start with a pelvic exam and an ultrasound to check endometrial thickness. If the lining looks thick or the bleeding is unexplained, the next step is an endometrial biopsy or a dilation and curettage (D&C). That tissue sample tells whether cells are simple hyperplasia (lower risk) or complex/atypical hyperplasia (higher risk for cancer).
Treatment depends on the type and your plans for fertility. For simple hyperplasia, a progesterone treatment — pills, an IUD that releases levonorgestrel, or injections — often reverses the thickening within months. Atypical hyperplasia is trickier: many doctors recommend a hysterectomy if you’re done having children, because the chance of cancer is higher. If you want to keep fertility, close monitoring and high-dose progestin therapy with frequent biopsies can be an option.
Follow-up matters. Even after treatment, doctors check the lining with repeat biopsies or ultrasounds until it returns to normal. Lifestyle steps help too: losing weight, treating insulin resistance, and managing PCOS reduce estrogen dominance and lower recurrence risk.
If you’ve had unusual bleeding, don’t wait. Ask your provider for a pelvic ultrasound and, if needed, an endometrial biopsy. Early answers make treatment simpler and protect your long-term health. For related reads on fertility, PCOS, and hormone treatments, check our guides on ovulation, letrozole vs clomiphene, and post-treatment follow-up.
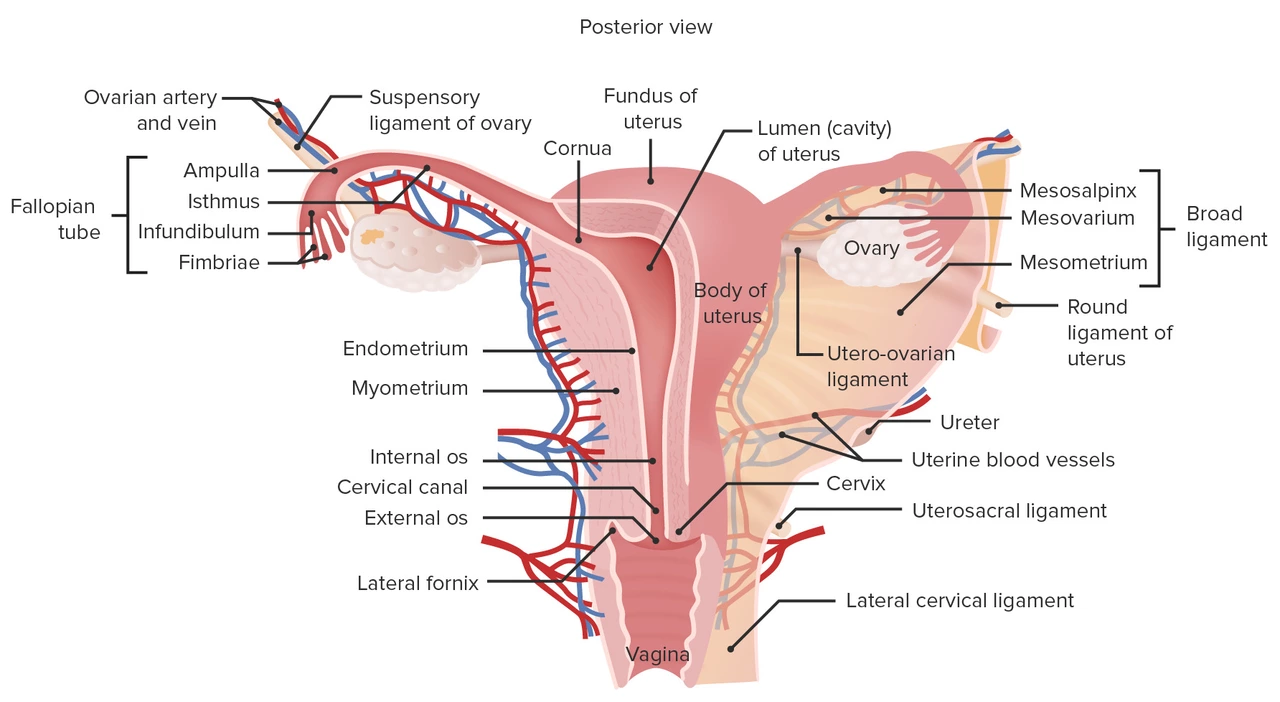
The Role of Endometrial Hyperplasia in Overgrowth of the Uterine Lining
- May, 6 2023
- Daniel Remedios
- 18 Comments
As a blogger, I've recently been researching the role of endometrial hyperplasia in the overgrowth of the uterine lining. Endometrial hyperplasia is a condition where the uterine lining thickens, which can be caused by an imbalance of hormones, particularly estrogen. This thickening can lead to heavy or irregular periods, and in some cases, can even cause infertility. It's important to monitor and treat endometrial hyperplasia, as it may increase the risk of developing uterine cancer. Overall, understanding and addressing endometrial hyperplasia is crucial for maintaining a woman's reproductive health.
