Diagnosing: Practical Tips for Understanding Tests and Symptoms
A clear diagnosis can change everything fast. If you’ve ever left a clinic confused by lab numbers or a vague note in your file, this page is for you. I’ll show simple ways to think about symptoms, what common tests actually tell you, and how to prepare for appointments so you get answers.
Start with what matters: symptoms. Write down when they started, what makes them better or worse, and any patterns. Short notes like “worse at night,” “after meals,” or “sharp pain when bending” help doctors narrow options. Don’t forget lifestyle details—sleep, stress, alcohol, and meds can change test results.
Next, know the common tests. Blood tests check things like infection, inflammation, kidney and liver function, and blood sugar. Imaging tests—X-ray, ultrasound, CT, MRI—show structure: fractures, fluid, or masses. ECG and echocardiogram look at heart rhythm and function. Each test answers a specific question, not everything at once.
Understand test results in plain terms. Numbers alone don’t tell the whole story. A slightly high liver enzyme may point to a minor issue or a medication effect; a very high number means urgent follow-up. Lab reports include reference ranges—think of them as a guide, not a verdict. If a result worries you, ask the provider: “How does this change the plan?”
Preparing for Tests and Appointments
Bring a short timeline of your symptoms, a current meds list, and any prior reports or images on a phone or USB. Ask about fasting rules before bloodwork and whether you should stop certain meds. Clear communication speeds diagnosis and avoids repeat tests.
Red Flags and Next Steps
Some signs need fast action: sudden severe chest pain, breathlessness, fainting, sudden weakness, severe bleeding, or confusion. If you see these, call emergency services. For non-urgent but persistent issues—ongoing pain, unexplained weight loss, or repeated abnormal labs—ask for follow-up testing or a referral to a specialist.
Second opinions matter. If a diagnosis feels incomplete, get another view. Different doctors order different tests and may spot something missed before. Keep copies of all results and summaries; it makes new consultations faster and clearer.
Use reliable sources to learn more—medical centers, specialty societies, and drug databases. Avoid symptom checkers as final answers; they’re useful for ideas but can mislead. Finally, stay engaged: ask questions, repeat back what you heard, and keep a record of next steps. That habit alone improves outcomes.
A few common pitfalls to avoid: running to tests without a clear question wastes time and money; stopping medications before talking to your doctor can cause harm; relying on a single test often misses the pattern a doctor needs. If symptoms come and go, ask for symptom-triggered testing or home monitoring — like blood pressure cuffs or glucose meters — so you capture the moment. Use photos or smartphone recordings for visible signs (rashes, tremors, swelling). These small actions give your provider concrete data and usually speed up getting the right diagnosis. Ask until you understand the next steps.
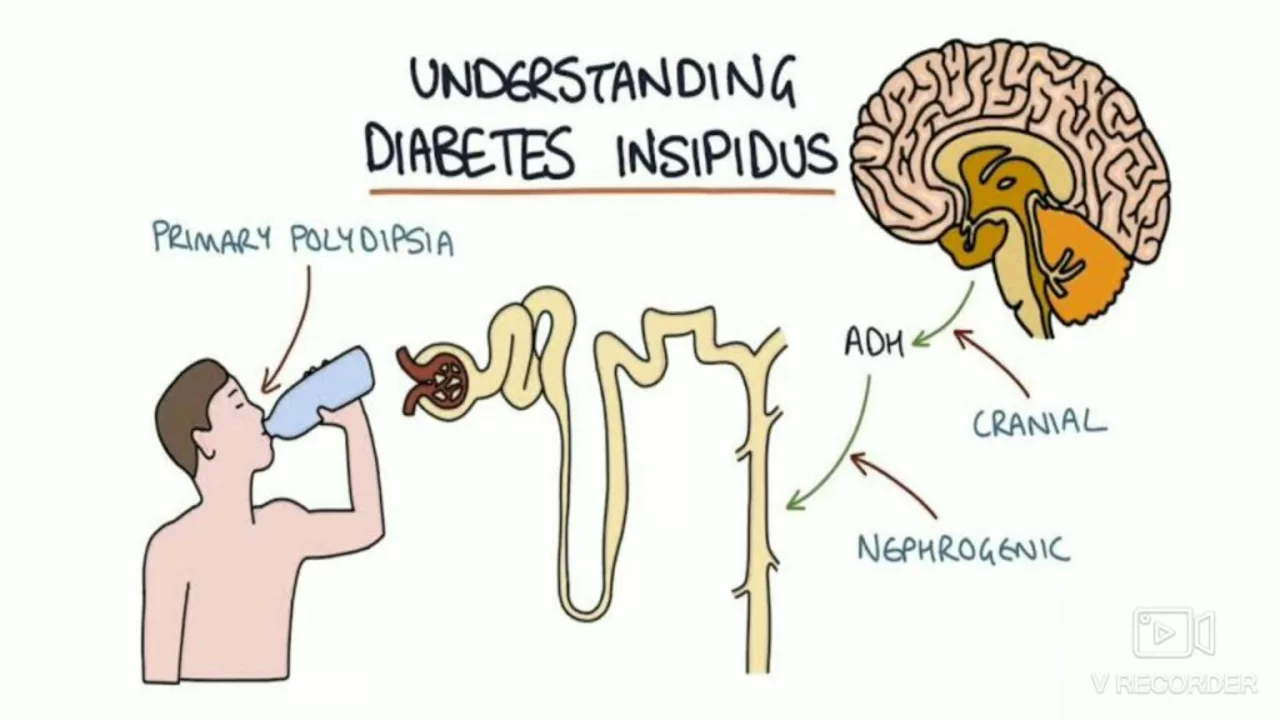
Diagnosing Central Cranial Diabetes Insipidus: Tests and Procedures
- Jul, 1 2023
- Daniel Remedios
- 16 Comments
In my recent exploration, I focused on the diagnostic processes involved in identifying central cranial diabetes insipidus. I found that doctors often perform blood and urine tests initially to check for low sodium levels and high urine output. Water deprivation tests and MRI scans are also used to confirm the diagnosis and assess the pituitary gland's condition. Desmopressin tests can then help to distinguish between central and nephrogenic diabetes insipidus. It's a detailed process, but crucial for ensuring accurate diagnosis and treatment.
