Smoking: Health Risks, How It Affects Medications, and Ways to Quit
One cigarette doesn't just stain fingers — it changes how your body handles drugs and heals. If you smoke, you should know two practical facts: smoking raises the risk of serious illnesses, and it can change the levels or effects of some medicines. That matters if you take prescriptions every day.
Why smoking matters for your health and medications
Smoking raises the chances of lung cancer, COPD, heart attack, stroke, and many other problems. It also speeds up certain liver enzymes (mainly CYP1A2). That means some drugs are broken down faster in smokers. Common examples include certain antipsychotics and theophylline. Faster breakdown can make a medicine less effective, so doctors may need to adjust doses if you smoke — or again if you quit.
If you stop smoking, drug levels can rise because the enzyme activity drops back. That can cause stronger effects or side effects unless your provider lowers the dose. Always tell your doctor and pharmacist about smoking habits before they change your meds.
Practical quitting options that work
There are four reliable approaches: nicotine replacement (patch, gum, lozenges), two prescription drugs (bupropion SR and varenicline), counseling, and a combination of these. Patches give steady nicotine. Gum or lozenges help short bursts of craving. Bupropion eases withdrawal and can lift mood. Varenicline reduces pleasure from smoking and cuts cravings. Combining counseling with medicine gives the best odds.
Small, clear steps help: pick a quit date, remove triggers (ashtrays, lighters), plan what to do when cravings hit (walk, chew gum, use a lozenge), and get support — a coach, friend, or quitline. If one method fails, try another. Many people need several attempts before they quit for good.
Worried about weight gain or mood swings? Talk to your clinician. Some medications used to stop smoking can affect mood, and some weight change is common — but the health gains from quitting are far bigger than these downsides.
What about vaping? Switching to e-cigarettes may reduce exposure to some toxins found in cigarette smoke, but vaping still carries risks and isn’t risk-free. If your goal is to quit nicotine altogether, plan an exit from vaping too.
On this site you’ll find useful related reads: check our articles about alternatives to bupropion, addiction treatments like naltrexone, and how certain drugs interact with alcohol and other substances. Use those posts to get a fuller picture before you adjust any treatment.
If you smoke and take medication, first step: tell your prescriber. If you want to quit, start with one clear plan — medicine, counseling, or both — and get support. Small changes today make a big difference for health and for how your medicines work.
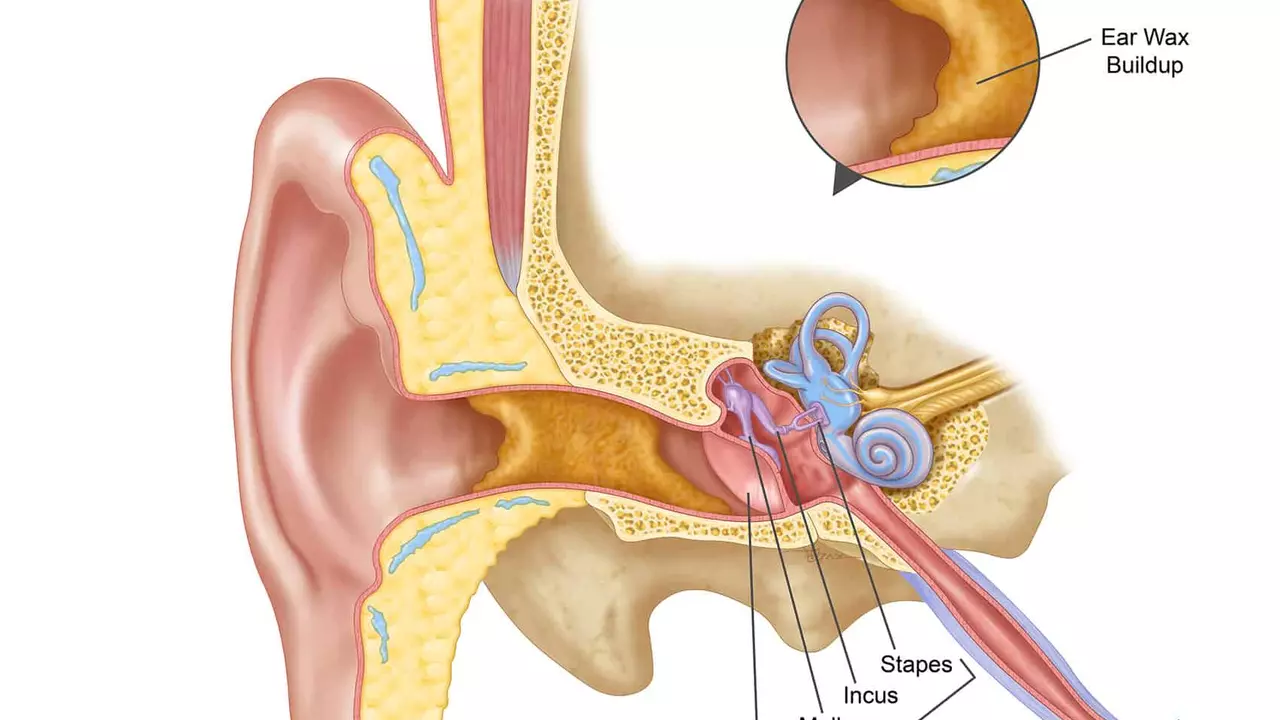
The Link Between Smoking and Ear Canal Infections
- Jun, 18 2023
- Daniel Remedios
- 12 Comments
As a blogger, I recently came across some interesting research showing a link between smoking and ear canal infections. It turns out that smoking not only affects our lungs but can also cause infections in our ears. The chemicals found in cigarettes can weaken our immune system, making it easier for bacteria and viruses to cause infections. Additionally, smoke can irritate the sensitive skin in our ear canals, leading to inflammation and increased risk of infection. Knowing this, I highly encourage everyone to consider quitting smoking to not only improve lung health but also protect their ears from infections.
