Betaxolol — what it does and when you might need it
Betaxolol is a beta-1 selective blocker used as an eye drop for glaucoma and as an oral pill for high blood pressure or angina. If your doctor prescribed betaxolol, you probably want to know how it helps, what to watch for, and simple tips to use it safely. This guide keeps things practical and easy to follow.
How betaxolol works and when it’s used
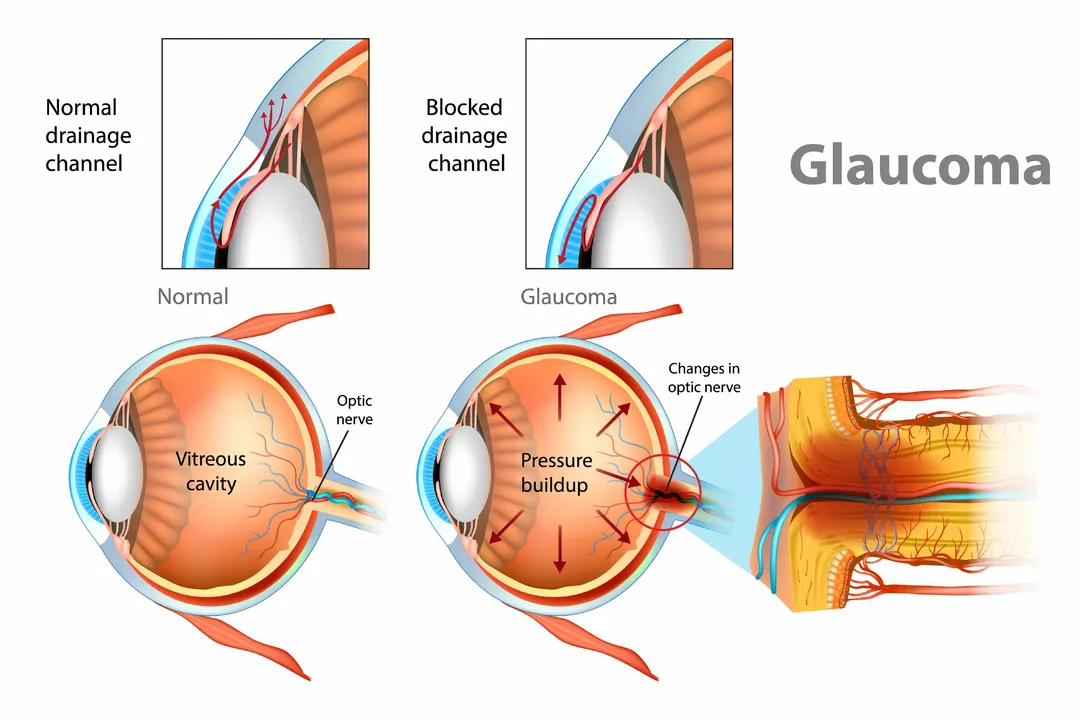
For glaucoma, betaxolol eye drops lower pressure inside the eye by slowing fluid production. Lower pressure protects the optic nerve and reduces the risk of vision loss. As a pill, betaxolol lowers heart rate and blood pressure by blocking beta-1 receptors in the heart, which helps with hypertension and chest pain.
Typical forms and doses: eye drops usually come as 0.25% or 0.5% solutions used once or twice daily, depending on your doctor’s plan. Oral betaxolol pills are often 10–40 mg once daily. Follow the exact instructions from your prescriber — don’t guess or mix dosing schedules.
Safety tips and common side effects
Most people tolerate betaxolol well, but a few things matter. Eye drops can cause mild stinging, blurred vision, or dry eyes right after use. If those symptoms last, tell your provider. With oral use, expect possible tiredness, slow heartbeat, dizziness, or cold hands and feet.
Important warnings: if you have asthma or serious COPD, betaxolol can make breathing worse — even though it’s more selective for the heart, it can still affect the lungs. People with slow heart rate, certain heart blocks, or uncontrolled heart failure should avoid it unless a cardiologist approves. Also, betaxolol can mask symptoms of low blood sugar (like a fast heartbeat), so people with diabetes need closer monitoring.
Drug interactions matter. Combining betaxolol with other heart medicines (like verapamil or diltiazem) can cause a very slow heart rate. Always tell your prescriber about all meds, supplements, and herbal products you take.
How to use drops well: wash your hands, tilt your head back, pull the lower eyelid to make a small pocket, squeeze one drop, close your eye for 1–2 minutes, and press gently at the inner corner to reduce systemic absorption. Wait five minutes before using another eye drop. Don’t wear contact lenses right after using drops unless your doctor says it’s fine.
Never stop betaxolol suddenly, especially if you use it for heart disease — stopping quickly can worsen angina or cause rebound blood pressure rise. If you want to stop, your doctor will usually taper the dose over days or weeks.
If you notice serious symptoms — trouble breathing, fainting, very slow pulse, or sudden vision changes — get medical help right away. For minor side effects, report them at your next visit and ask about dose changes or alternatives.
Simple checks to keep safe: monitor blood pressure and pulse regularly, bring a list of all medicines to appointments, and store eye drops at room temperature away from light. Talk to your doctor before pregnancy, breastfeeding, or major surgery.
Got questions about your betaxolol plan? Ask your pharmacist or prescriber — they can adjust dose, timing, or suggest safer alternatives based on your health. Small steps and clear communication keep treatment effective and safe.
Betaxolol: How to Maximize Its Effectiveness in Glaucoma Treatment
- Apr, 27 2023
- Daniel Remedios
- 10 Comments
As a glaucoma patient, I've found that betaxolol is an effective medication for managing my condition. To maximize its effectiveness, I make sure to follow my doctor's prescribed dosage and administration instructions carefully. Additionally, I've learned the importance of regular eye exams to monitor my intraocular pressure and overall eye health. I also try to maintain a healthy lifestyle, including proper diet and exercise, to support my glaucoma treatment. Finally, I always communicate with my healthcare team about any side effects or concerns to ensure the best possible outcome with betaxolol therapy.
