Alendronate: A Practical Guide to Uses and Safe Use
Alendronate (often known by brand name Fosamax) is a common prescription for preventing and treating osteoporosis. It slows bone loss, lowers fracture risk, and is usually prescribed to postmenopausal women, men with low bone density, or people on long-term steroids. This page gives clear, practical tips on how it works, how to take it, side effects to watch for, and simple precautions you can use every day.
How it works: Alendronate belongs to a class called bisphosphonates. It sticks to bone and slows the cells that break bone down. That helps build stronger bone over months and years. You won’t feel changes day to day, but bone density tests usually show improvement after a year.
How to take alendronate safely
Take alendronate first thing in the morning, with a full glass (240 ml) of plain water. Don’t eat, drink anything else, or take other supplements or meds for at least 30 minutes after the pill — some doctors recommend waiting 60 minutes for weekly doses. Stay upright while you wait; lying down raises the risk of throat or stomach irritation. Swallow the tablet whole; don’t chew or dissolve it.
Different schedules exist: there are daily and weekly tablets. Your doctor will pick the right dose based on your bone density, age, and health. If you miss a dose, follow the prescription leaflet or ask your pharmacist — don’t double up without guidance.
Side effects, risks, and who should avoid it
Common side effects include stomach upset, heartburn, and muscle pain. Most people tolerate alendronate well, but a few rare problems deserve attention. Severe reflux, difficulty swallowing, persistent jaw pain, or new thigh or groin pain should prompt an immediate call to your doctor — these can signal serious but uncommon effects like esophagus injury, osteonecrosis of the jaw, or unusual femur fractures.
Avoid alendronate if you have low esophageal motility, active stomach ulcers, or inability to sit or stand upright for 30–60 minutes. People with very low kidney function often need a different treatment. Tell your doctor about calcium and vitamin D supplements; timing matters because calcium reduces alendronate absorption. If you’re pregnant or breastfeeding, don’t take it unless your clinician says it’s necessary.
Monitoring and alternatives: Your doctor will check bone density with DXA scans and review calcium and vitamin D. If alendronate isn’t suitable, other options include risedronate, ibandronate, denosumab, or lifestyle changes such as weight-bearing exercise, adequate calcium and vitamin D, and quitting smoking.
Simple tips: take a calcium supplement at a different time, keep dental checkups while on treatment, report any new bone pain immediately, and ask about drug holidays after five years with your doctor.
Bottom line: Alendronate can be effective when used correctly. Follow dosing rules, report worrying symptoms fast, and keep routine bone checks. If you have questions about interactions or long-term use, ask your healthcare provider — small changes in how you take the drug make a big difference for safety and results.
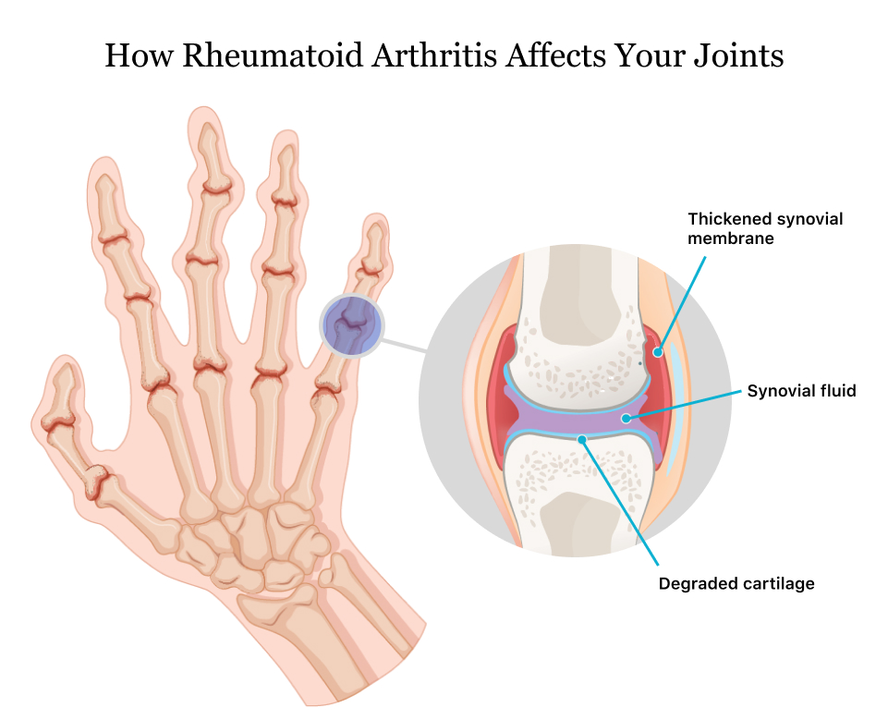
Alendronate and Rheumatoid Arthritis: Can it Help?
- May, 21 2023
- Daniel Remedios
- 12 Comments
In my recent research on rheumatoid arthritis treatments, I came across a medication called Alendronate. This drug, typically used for osteoporosis, has shown potential benefits in managing rheumatoid arthritis symptoms. Studies have indicated that Alendronate may help reduce inflammation and bone erosion, which are common issues for those with rheumatoid arthritis. However, more research is needed to fully understand the drug's effectiveness and long-term effects on rheumatoid arthritis patients. It's crucial for individuals to consult with their healthcare provider before considering Alendronate or any new treatment.
